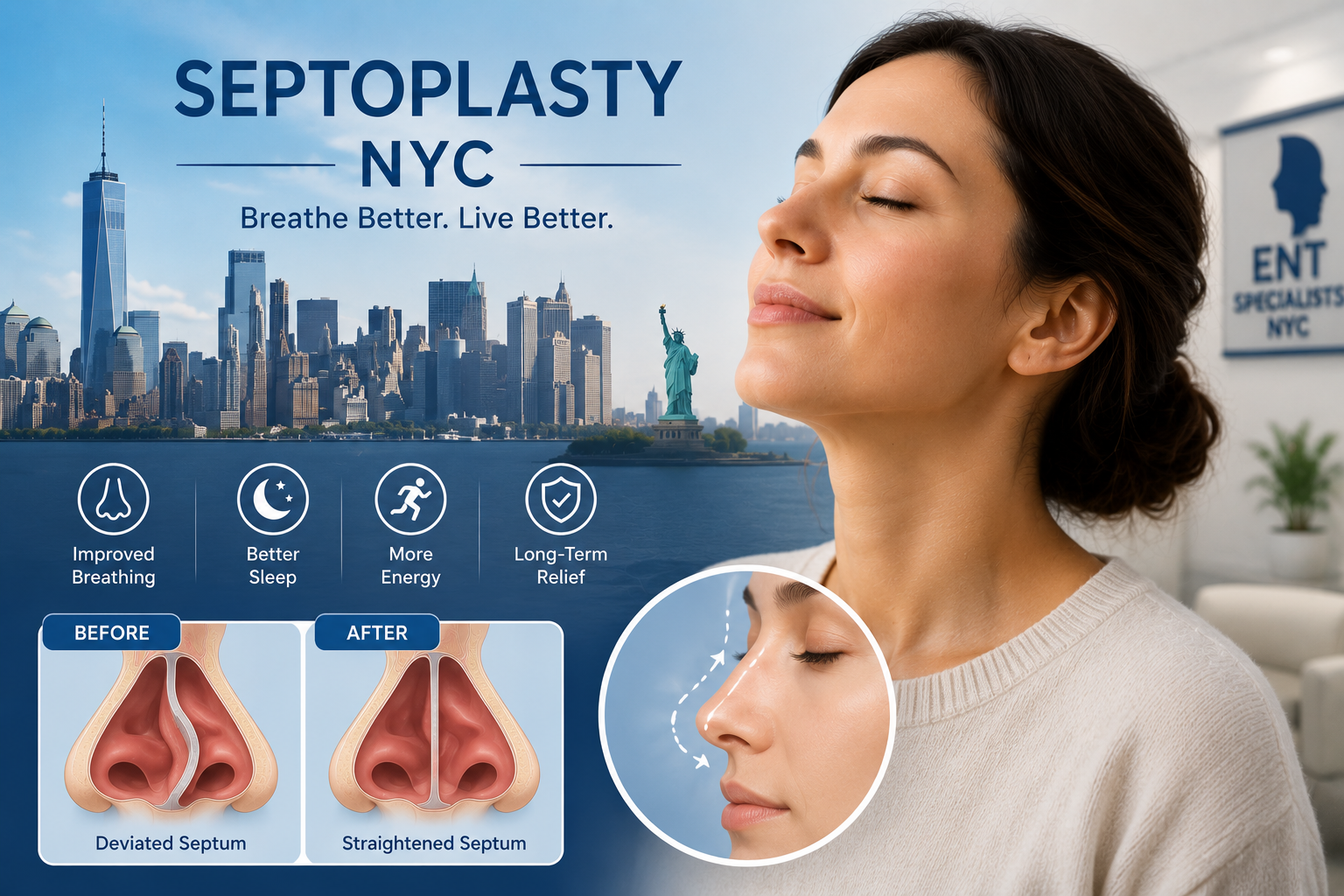
Septoplasty NYC:
Breathe Freely Again
with Dr. Mourad
Struggling with a deviated septum, chronic congestion, or breathing difficulties affecting every aspect of your life? Dr. Mourad offers expert septoplasty surgery in NYC that restores both function and aesthetic harmony — with dual board-certified precision.
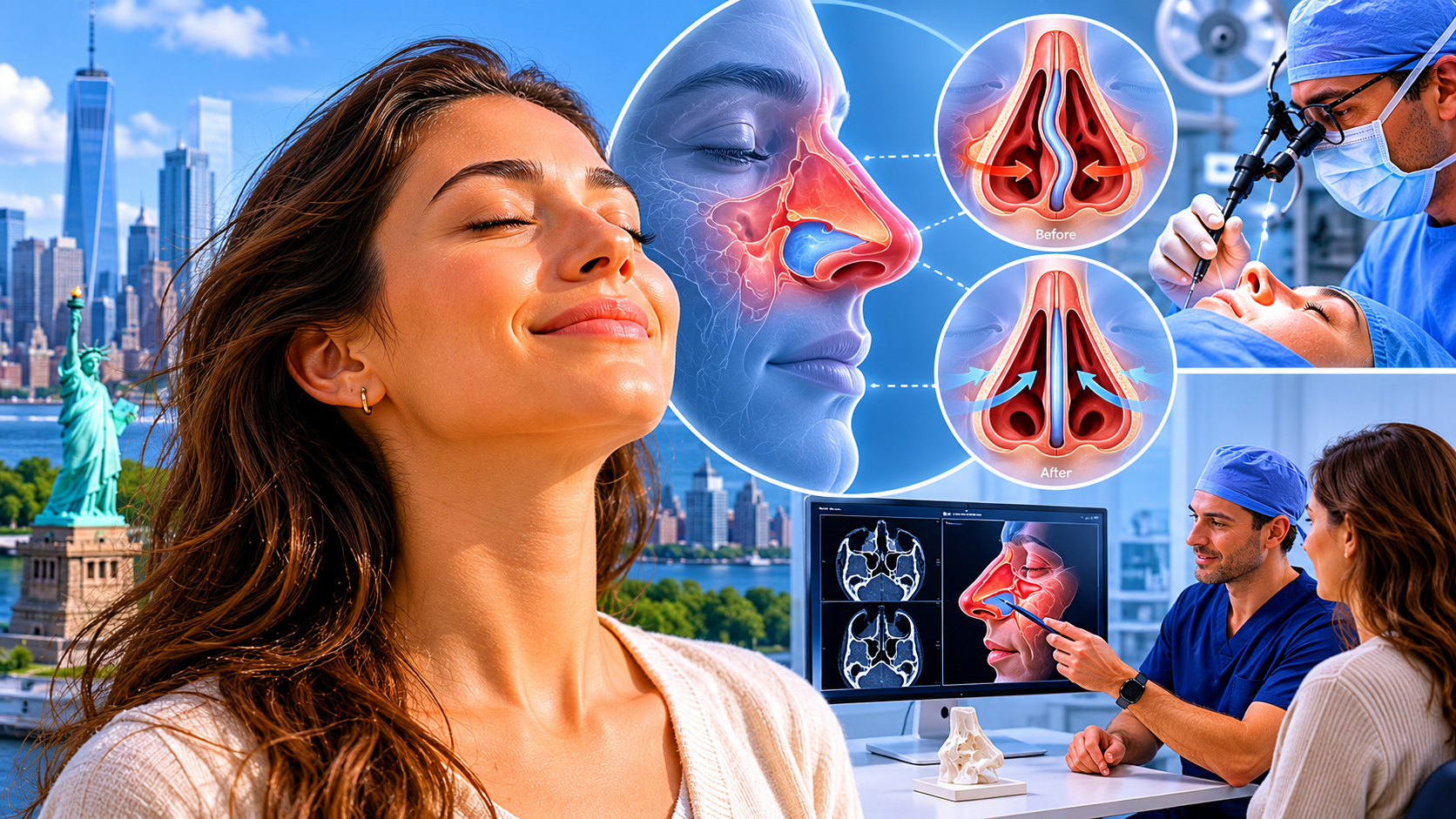
Septoplasty Expertise
Dual Board-Certified
Facial Plastic & Reconstructive Surgery and Otolaryngology (ENT)
AAFPRS Director
American Academy of Facial Plastic & Reconstructive Surgery
ENT Specialist
Airway, breathing & nasal structure treated alongside aesthetic concerns
923 Fifth Avenue
Suite 1A, Manhattan — Upper East Side, New York City
Expert Care
Discover Relief: The Emotional Impact of Septoplasty
In my Manhattan practice, I’ve seen how breathing difficulties can impact every facet of a patient’s life. It’s not just about feeling congested or snoring at night. It’s about the frustration of not being able to take a full, satisfying breath, the anxiety that comes with feeling like you’re constantly gasping for air, and the isolation that can stem from avoiding social situations because you’re embarrassed by your breathing issues. These are real, tangible challenges that many face daily.
What I tell patients in consultation is that septoplasty isn’t just a procedure — it’s a pathway to relief. For those grappling with a deviated septum, the promise of breathing freely and living without the burden of constant congestion is life-changing. Nearly a decade of practice has shown me that improved breathing can enhance not just physical health but emotional well-being, too. Imagine waking up feeling refreshed, participating in activities you love without the constant struggle for air, and engaging with the world around you with renewed energy.
Yet, with the prospect of surgery comes fear. “I’m terrified of looking ‘done’ or unnatural,” some say. It’s a valid concern. No one wants to lose what makes them uniquely themselves. My philosophy is rooted in structural refinement and preservation of identity. I aim for results that enhance, rather than alter, the essence of who you are. In my practice in New York City, we focus on achieving functional and aesthetic harmony — never aggressive reduction or that dreaded “wind-tunnel” look.
Some patients worry, “Will I lose what makes me look like me?” The answer is no. The goal is to refine, not redefine. My ENT background allows me to treat airway, breathing, and structure as a comprehensive unit, ensuring that we address both function and form. For those who’ve had surgery before that didn’t go well, there is hope. Revision cases are a significant part of my practice — patients come to me when others have said no, and I’m committed to finding solutions where others see none.
Why Choose Dr. Mourad for Your Septoplasty

Experience, Expertise & a Philosophy of Preservation
When considering septoplasty surgery in NYC, the choice of surgeon is paramount. In my practice in Manhattan, I often tell patients that the surgeon’s expertise makes all the difference — not just in outcomes, but in the entire experience. With dual board certification from the American Board of Facial Plastic & Reconstructive Surgery and the American Board of Otolaryngology, I bring a unique blend of skills to the table. This comprehensive background allows me to treat both the functional and aesthetic aspects of nasal surgery with precision and care.
Dr. Mourad is not your average surgeon. In fact, other surgeons refer their most challenging cases to me — those complex situations where others have said no. This isn’t just a testament to my technical skill but to my philosophy of patient care. As an AAFPRS Director, I stay at the forefront of surgical advances and contribute to the educational landscape, ensuring that my approach is both innovative and grounded in the latest research. My textbook authorship further reflects my commitment to advancing the field.
Patients often express fears about surgery: “Will I lose what makes me look like me?” or “I’m terrified of looking ‘done’ or unnatural.” These concerns are valid. My approach is centered on structural refinement and preservation of identity. I don’t believe in aggressive reductions or creating a “wind-tunnel” appearance. Instead, I aim to enhance your natural features, ensuring the result is harmonious and true to who you are.
In my decade of practice, I’ve found that the most consistent pattern is achieving functional improvement without sacrificing aesthetics. Whether it’s a primary septoplasty or a complex revision, my focus is on delivering results that look natural and feel right — something my dual expertise in facial plastic surgery and ENT uniquely qualifies me to do.
- Dual Board-Certified: Facial Plastic Surgery & Otolaryngology (ENT)
- AAFPRS Director — leading surgical innovation nationally
- Expert in primary & revision septoplasty, open & closed techniques
- Face-exclusive practice for unmatched nasal precision
- Trusted by other surgeons for the most complex referrals
Ideal Candidates for Septoplasty
In my practice in New York City, the question of who truly benefits from septoplasty frequently arises. It’s not just a matter of having a deviated septum — it’s about understanding the real impact on your daily life. For many, a deviated septum is a constant battle with blocked nasal passages, chronic congestion, and the frustration of never quite catching your breath. If you find that your nasal obstruction affects your sleep, your exercise routines, or even your social interactions, you might be an ideal candidate for septoplasty surgery in NYC.
Breathing & Functional Issues
Septoplasty is about more than just straightening a septum — it’s about improving your overall quality of life. Those who suffer from recurrent sinus infections, frequent nosebleeds, persistent headaches, or sleep disturbances may find relief through this procedure. In my decade of practice, I’ve observed that patients often report a marked improvement in their energy levels and a reduction in fatigue once they can breathe more freely. If conservative treatments have failed to provide lasting relief, surgery is often the right next step.
Aesthetic & Functional Harmony
There’s an aesthetic angle as well. My ENT background enables me to address both structural and cosmetic concerns simultaneously — you won’t just breathe better, you’ll feel more confident about your appearance too. My approach is rooted in preserving your unique features. The goal is never to alter who you are but to enhance your natural structure, creating balance without compromising identity.
Revision Septoplasty Candidates
Ideal candidates also include those who have previously undergone nasal surgery without satisfactory results. Revision cases are particularly complex, but they’re also where my skills are most valuable. If you’ve had surgery before that didn’t resolve your issues — or perhaps created new problems — it’s worth considering a consultation. Other surgeons often refer these challenging cases to me, trusting in my ability to find solutions where others might not. Candidates should be in good general health; a thorough consultation will confirm whether septoplasty is the right and safe option for you.


Types of Septoplasty Performed by Dr. Mourad
In my decade of practice, I’ve encountered a wide range of nasal conditions, each requiring a tailored surgical approach. Septoplasty isn’t a one-size-fits-all solution — it’s a spectrum of techniques designed to address your specific anatomy, symptoms, and surgical history.
Primary Septoplasty
Primary septoplasty is often the first surgical intervention for those suffering from a deviated septum. This procedure aims to correct the nasal septum’s alignment, improving airflow and alleviating symptoms like chronic congestion, headaches, or sleep disturbances. When performed correctly, primary septoplasty offers a significant improvement in both function and comfort — without compromising your natural appearance.
Revision Septoplasty
Revision septoplasty corrects or refines the results of a previous nasal surgery. Patients often come to me after unsatisfactory outcomes elsewhere, carrying the burden of disappointment and hope for resolution. Revision cases are inherently more complex — scar tissue, altered anatomy, and previous surgical changes all add layers of complication. This is where my dual board certification and ENT expertise become invaluable.
Open Septoplasty
Open septoplasty involves a small incision on the columella, providing unparalleled visibility of the nasal structures. This allows for precise correction of complex issues — particularly beneficial when significant structural changes are needed or when previous surgeries have altered the nasal anatomy. For complex or revision cases, the open approach offers the flexibility to address intricate deformities with accuracy.
Closed Septoplasty
Closed septoplasty involves incisions made within the nostrils, leaving no visible external scars. This less invasive approach is typically employed when deviations are less severe, offering a quicker recovery time. For patients concerned about scarring or who require minor corrections, closed septoplasty can be an excellent option — though it requires deep nasal anatomy knowledge to achieve precise results.
Still struggling to breathe freely?
Book a no-commitment consultation and get an honest, expert opinion on your septoplasty options.

Open vs. Closed Septoplasty: Choosing the Right Technique
When considering septoplasty surgery in NYC, understanding the surgical approach — whether open or closed — is crucial. Each method has distinct advantages, and the choice depends on individual needs and anatomical considerations. In my Manhattan practice, I guide patients through these options, ensuring they comprehend the nuances involved in their surgical plan.
Open septoplasty involves a small incision made on the columella, the tissue between the nostrils. This approach provides unparalleled visibility of the nasal structures, allowing for precise correction of complex issues. It’s particularly beneficial for cases where significant structural changes are needed or when previous surgeries have altered the nasal anatomy. The open approach offers the flexibility to address intricate deformities with accuracy, making it a preferred choice for complex or revision cases.
Closed septoplasty involves incisions made within the nostrils, leaving no visible scars. This approach is less invasive and is typically employed when the deviations are less severe. For patients concerned about scarring or who require minor corrections, closed septoplasty can be an excellent option, offering a quicker recovery time. The challenge with this technique lies in the limited visibility, which necessitates a deep understanding of nasal anatomy — a benefit of my dual board certification.
Choosing between open and closed septoplasty isn’t a one-size-fits-all decision. The best approach is the one that aligns with your specific anatomical needs and goals. During our consultation, we conduct a comprehensive evaluation considering the severity of the deviation, any previous surgeries, and the desired aesthetic outcome. Patients often worry: “Will an open approach make me look different?” The goal of any septoplasty — open or closed — is to enhance function while preserving your natural appearance.
What to Expect During Your Consultation
When you step into my Manhattan office for a septoplasty consultation, it’s the beginning of a journey tailored to your unique needs. The consultation process is not just a formality — it’s an essential part of crafting a treatment plan that aligns with both your functional and aesthetic goals. After nearly a decade of practice, I’ve learned that a successful outcome starts with understanding your specific concerns and aspirations.
In my practice in New York City, the consultation is a comprehensive assessment. We’ll start by discussing your medical history in detail, including any previous nasal surgeries or ongoing health conditions. My dual board certification in facial plastic surgery and ENT means I’ll evaluate both the cosmetic and functional aspects of your nose, ensuring we address any airway issues alongside aesthetic concerns. One of the most common fears patients express is the worry about looking unnatural — “I’m terrified of looking ‘done’,” many say. This consultation is your opportunity to voice these concerns.
The clinical assessment will include a physical examination of your nasal structure. Using advanced imaging techniques, we’ll visualize the internal and external aspects of your nose. This allows me to pinpoint any deviations or obstructions affecting your breathing and to design a surgical plan that addresses these issues effectively. We’ll also discuss the different surgical approaches — open versus closed septoplasty — and which might be most suitable for your situation.
Recovery is another key topic we’ll cover. I’ll provide a detailed overview of the recovery timeline, including what to expect in terms of swelling, discomfort, and downtime. Throughout the consultation, my goal is to build trust and ensure you’re comfortable with the proposed plan. Surgery isn’t just about technical skill — it’s about understanding and aligning with your vision. You will leave with a clear understanding of your diagnosis, your options, and what to realistically expect.
The Septoplasty Procedure: Techniques and Anesthesia
As we move forward into the specifics of the septoplasty procedure itself, let’s delve into what you can expect on the day of surgery. Septoplasty is typically performed as an outpatient procedure, allowing you to return home the same day. The duration generally ranges from one to three hours, depending on the complexity of the case — whether it’s a straightforward primary septoplasty or a more involved revision.
The procedure begins with anesthesia. In my practice, we offer two main types: local anesthesia with sedation, or general anesthesia. Local anesthesia with sedation numbs the nasal area and uses a sedative to relax you, while general anesthesia ensures you’re completely asleep during the procedure. Each option is carefully considered during your consultation, with your safety and comfort as the primary focus.
Once anesthesia is administered, we proceed with either an open or closed surgical approach. In open septoplasty, a small incision is made on the columella, allowing direct access to the nasal structures with unparalleled visibility — especially beneficial in complex or revision cases. In closed septoplasty, incisions are made within the nostrils, leaving no external scars, and offering a quicker recovery. During the procedure, the deviated portions of cartilage and bone are carefully repositioned, trimmed, or reshaped to improve airflow. In some cases, cartilage grafts may be employed to support or enhance the nasal structure.
After the procedure, you’ll spend time in a recovery area monitored by my team as the anesthesia clears. You’ll receive detailed post-operative instructions tailored to your specific needs, aiding in a successful recovery. Most patients return home the same day, with follow-up appointments scheduled to monitor healing and progress. Post-procedure care doesn’t end when you leave the facility — I’m committed to being available for any questions or concerns that arise as you recover.
Ready to finally breathe freely again?
Patients from the tri-state area and beyond trust Dr. Mourad for expert septoplasty and nasal care.
Recovery Timeline: What to Expect Post-Septoplasty
Days 1–3: Immediate Post-Op Phase
The first few days post-surgery are all about rest and gentle care. You’ll likely experience swelling, congestion, and some discomfort — these are normal and expected. Elevating your head while sleeping can significantly reduce swelling, and using cold compresses can offer relief. Pain is typically mild to moderate, managed with prescribed medications — most patients describe it as a sense of pressure rather than sharp pain. You’ll have nasal packing or splints in place to support the new structure; avoid blowing your nose or any strenuous activities during this time.
Days 4–7: Early Healing
As you move into the latter part of the first week, you’ll notice a gradual decrease in swelling and bruising. Many patients feel well enough to resume very light activities, though I advise against returning to work or any rigorous exercise. Your follow-up appointment will likely be scheduled around this time, where I’ll assess your healing progress and remove any packing or splints. Patients often express concerns about their appearance during this stage — I remind them that swelling is temporary, and patience is key.
Week 2: Transition Period
By the second week, most of the bruising will have faded, and the swelling will continue to diminish. Many patients feel comfortable enough to return to work, provided their job doesn’t involve physical exertion. You’ll start to notice improvements in breathing, although nasal congestion may still be present due to internal swelling — this will gradually resolve. Keeping your nasal passages moist with saline sprays can aid in this process.
Weeks 3–4: Steady Improvement
As you approach the one-month mark, you’ll see significant improvements in both function and appearance. The majority of swelling will have subsided, and your breathing should feel noticeably better. Many patients begin to see the subtle refinements in their nasal shape as the final results start taking form. You can gradually reintroduce more physical activities, though I advise against contact sports or activities posing a risk of facial injury until I’ve confirmed healing is sufficiently advanced.


Month 2–3: Settling In & Long-Term Results
In the months following surgery, your nose will continue to refine itself. The subtle changes that occur during this period contribute to the final outcome. By the three-month mark, most patients report a marked improvement in breathing and a more harmonious nasal profile — this is when you’ll truly start to appreciate the balance between function and aesthetics that septoplasty offers. Complete healing can take up to a year, with the most noticeable changes occurring in the first three months. It’s essential to maintain realistic expectations and trust in the process.
In the long term, the benefits of septoplasty extend beyond the physical. Patients often report a newfound confidence and an improved quality of life — breathing freely leads to better sleep, increased energy, and a greater ability to engage in activities you love. A common concern is, “Will I still look like me?” With a focus on structural refinement and preservation of identity, the goal is always to enhance your natural features, not alter them.
Cost and Value: Understanding Your Investment
Septoplasty is more than a cosmetic enhancement — it’s a functional necessity for many. The investment in septoplasty is an investment in your future health and happiness. The expertise of the surgeon, the complexity of your specific case, and the level of care provided all factor into the overall expense. “Is it worth it?” patients ask. In nearly a decade of practice, I’ve seen how transformative this surgery can be — the benefits extend beyond the physical, impacting emotional and social well-being.
Insurance often plays a role in covering septoplasty, particularly when the procedure is deemed medically necessary. If your deviated septum is causing significant breathing issues, there’s a strong possibility that insurance will cover a portion of the surgery. In my practice, we assist patients in navigating these conversations with their provider, ensuring you have a clear understanding of your benefits and potential out-of-pocket costs.

Who Should Avoid Septoplasty
While septoplasty can offer significant relief for many, it’s not the right path for everyone. In my practice in New York City, I emphasize that a thorough clinical assessment is crucial to determine if this procedure aligns with your health needs and lifestyle. I will always tell you honestly if surgery is not the right course of action — transparency is foundational to my practice.
I advise against septoplasty for individuals with uncontrolled medical conditions such as severe cardiovascular issues, poorly managed diabetes, or bleeding disorders, as these conditions significantly increase surgical risks. Those on blood-thinning medications may need to adjust their regimen in collaboration with their primary care physician before proceeding. Smokers also face unique challenges — nicotine impairs healing and increases the risk of infection; I strongly encourage cessation before undergoing septoplasty.
Age is another consideration. The nasal structure continues to develop through adolescence, and performing surgery too early can impact natural growth. For teenagers, I typically recommend waiting until the nasal structure is more mature — usually around the mid to late teens — unless there is a compelling medical reason. Mental health is also a critical aspect: patients with unrealistic expectations or those struggling with body dysmorphic disorder may not find satisfaction with outcomes, and psychological counseling may be beneficial before proceeding.
Those with a history of poor wound healing or excessive scarring — conditions like keloids or hypertrophic scars — may need to reconsider septoplasty, as these can affect cosmetic results. If evaluations indicate the nasal deviation is not significant enough to warrant surgery, my role is to give you an honest clinical assessment — not to recommend surgery simply because you’ve asked for it. A comprehensive consultation will determine the right path forward.
What Our Patients Say
Frequently Asked Questions
Honest, expert answers to the questions Dr. Mourad hears most often about septoplasty — because informed patients make the best decisions.
Contact Us- How is septoplasty different from rhinoplasty?
Septoplasty and rhinoplasty are often mentioned together, but they serve different purposes. Septoplasty focuses on correcting a deviated septum to improve breathing. Rhinoplasty, however, is primarily cosmetic, altering the nose’s appearance. In my practice in New York City, I often perform these surgeries together, addressing both function and aesthetics. Patients frequently ask about this distinction, especially those seeking a balance between breathing improvement and cosmetic refinement.
- What should I expect during recovery?
Recovery is a crucial part of the process. In the initial days post-surgery, expect some swelling and congestion — natural responses as your body heals. Many patients are surprised at how manageable the discomfort is, and I ensure you have a clear plan for managing any pain. By the end of the first week, most find their breathing significantly improved, although full results evolve over several months. Recovery isn’t just physical; it’s a time to embrace the changes and newfound ease in breathing.
- Are there risks with septoplasty?
Every surgical procedure carries risks, and septoplasty is no exception. Common concerns include bleeding, infection, or an unsatisfactory outcome. However, with my dual board certification and extensive experience, these risks are minimized. I emphasize the importance of following post-operative care instructions to reduce complications. My role is to ensure you’re informed and comfortable with every aspect of your care.
- How long before I see results?
Patience is key. While you’ll notice breathing improvements shortly after surgery, the nose continues to refine over several months. Swelling subsides gradually, revealing the final shape and function. Patients often tell me that the wait is worthwhile, as they experience both enhanced breathing and subtle aesthetic improvements that align with their natural features.
- Will I look “done” or lose my identity?
This is a common fear. My philosophy centers on preserving identity, not altering it. The goal is to enhance your natural features subtly. I reassure patients that my approach avoids drastic changes, focusing instead on structural refinement. In nearly a decade of practice, my aim has always been to ensure you look like yourself — only refreshed and more at ease.
- Can septoplasty help with sleep apnea?
Yes, for some patients, septoplasty can alleviate symptoms of sleep apnea. By correcting nasal obstructions, airflow improves, potentially reducing apnea episodes. It’s important to discuss your specific condition during our consultation to determine if septoplasty could benefit your sleep health.
- What if my previous surgery didn’t go well?
Revision septoplasty is a significant part of my practice. Many come to me disheartened by past surgeries, fearful of further disappointment. With my expertise in complex cases, I often find solutions where others cannot. The key is a thorough evaluation and realistic goal setting. My commitment is to restore both function and confidence.
- How do I know if insurance will cover my septoplasty?
Insurance coverage often hinges on whether the procedure is deemed medically necessary. If your deviated septum impacts your breathing, there’s a strong case for coverage. We assist in navigating these discussions with your provider, ensuring you have a clear understanding of your benefits and potential out-of-pocket costs.
- How soon can I return to normal activities?
While individual experiences vary, most patients resume light activities within a few days. I advise avoiding strenuous exertion for a couple of weeks to ensure optimal healing. My team and I provide detailed guidelines tailored to your lifestyle, ensuring a smooth transition back to your daily routine.
- Can septoplasty be combined with other surgeries?
Absolutely. It’s common to combine septoplasty with cosmetic procedures like rhinoplasty to address both functional and aesthetic goals simultaneously. This approach not only saves time but ensures a harmonious outcome. During your consultation, we’ll explore all options to create a tailored plan that meets your needs.

The Most Important Step: Your Expert Consultation
In my Manhattan practice, every consultation is a genuine clinical assessment — not a sales conversation. This allows us to understand your symptoms, evaluate your nasal anatomy, and determine what is realistically achievable through surgery or other interventions.
If you’re considering septoplasty surgery in NYC, I invite you to experience this expert evaluation. Whether you’re dealing with a deviated septum, contemplating revision surgery, or simply looking for an honest answer about your options, this is the right first step.


