How to Choose the Best Facelift Surgeon Near You: A Practical, Evidence‑Based Guide
February 18, 2026
A great facelift can be life-changing—and it’s one of the most technically demanding procedures in aesthetics. Results depend as much on a surgeon’s judgment, anatomical know‑how, and safety systems as they do on the specific technique. So choosing “the one” isn’t just about reviews or price. It’s about understanding the landscape, confirming credentials, evaluating clinical quality, and making sure the practice runs on patient safety and ethics.
Below is a clear, evidence‑based framework to help you choose with confidence.
Below is a clear, evidence‑based framework to help you choose with confidence.
Define Your Goals and Understand Facelift Fundamentals
Before you book consults, get clear on what you want—and what a facelift actually does. Knowing the basics makes it easier to assess recommendations.
Procedure spectrum and indications:
Procedure spectrum and indications:
- Deep-plane facelift: Repositions the SMAS and deeper retaining ligaments as one unit. Often addresses midface (cheek) descent, jowling, and deep nasolabial folds with natural pull vectors and strong longevity. Requires advanced expertise.
- SMAS facelift (plication or imbrication): Tightens or repositions the SMAS layer to sharpen the jawline and lower face. Widely used, versatile, and effective—especially for jowls and lower face contour.
- Mini-lift: Smaller incisions and limited dissection. Helpful for mild laxity or touch-ups, but typically less durable and less impactful on the neck.
- Neck lift: Targets neck bands, submental fullness, and the cervicomental angle. May include platysmaplasty (anterior corset or lateral suspension) and, when indicated, reduction of subplatysmal fat, digastric muscle prominence, or camouflage of the submandibular gland.
- Adjunctive procedures: Fat grafting (to replenish volume in cheeks, temples, pre‑jowl sulcus), skin resurfacing (CO2/Erbium lasers, peels) for texture and fine lines, plus neuromodulators or energy devices for maintenance.
- Ideal candidates have good skin quality, realistic expectations, and defined signs of facial aging—think malar descent, jowl formation, and neck banding.
- Factors such as sun damage, ligament laxity, and deep neck anatomy affect the approach and outcome.
- Medical issues (e.g., hypertension, anticoagulation, diabetes, nicotine use) influence risk and timing; optimize them first for safer surgery and better results.
- The art is in the vectors. Skilled surgeons tailor SMAS management, platysma strategy, and skin redraping to restore structure—without distortion.
- Incisions should preserve the sideburn, respect the hairline, and curve naturally around auricular anatomy to minimize visible scars and avoid “pixie‑ear” deformity.
- Longevity varies by technique, tissue quality, and lifestyle. Many patients enjoy refreshed contours for 8–12 years or more, though aging rolls on.
- Maintenance matters: skincare, sun protection, neuromodulators, energy devices, and occasional touch‑ups help. Staged treatments (e.g., resurfacing or fat grafting) can refine results over time.
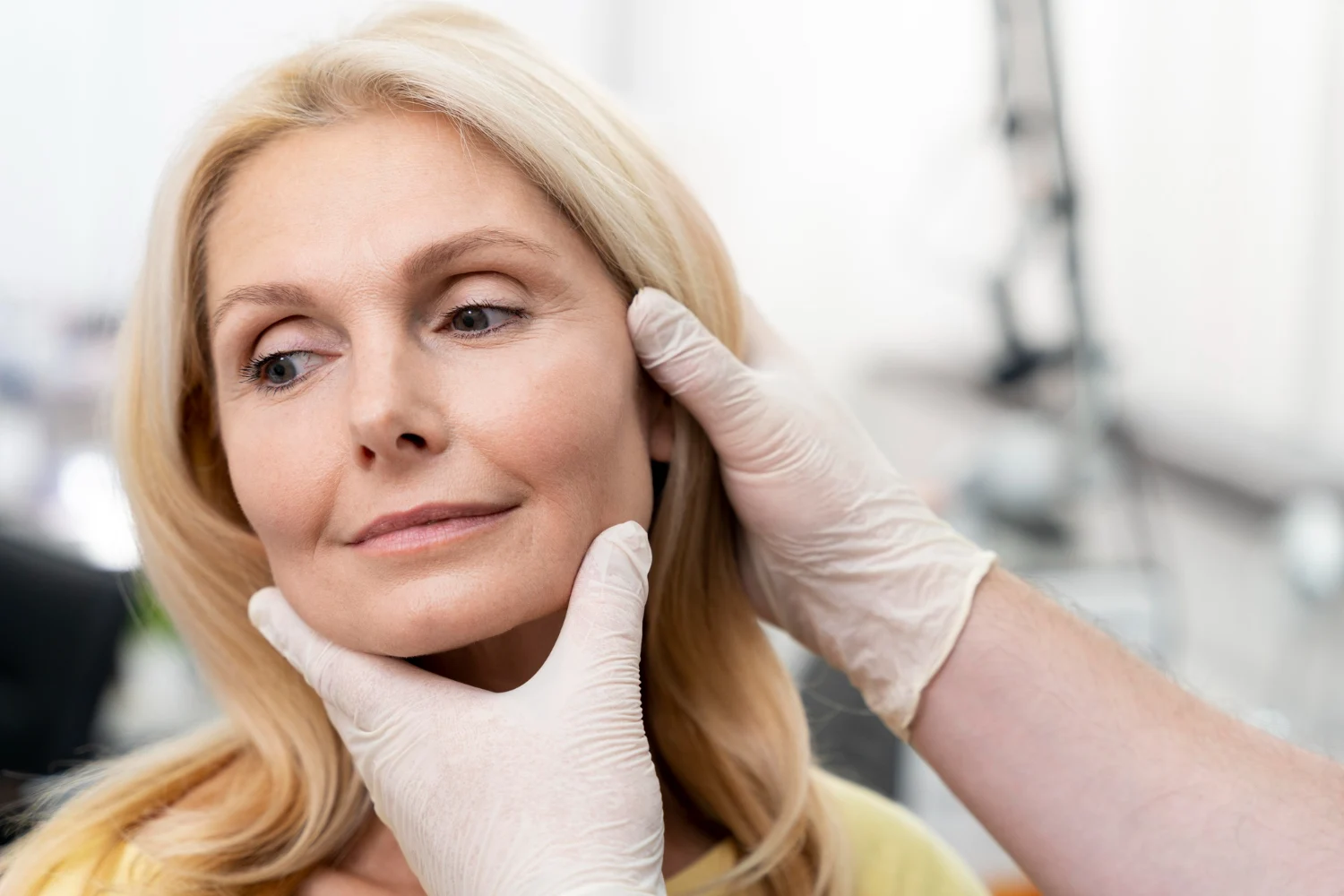
Verify Credentials, Training Pathways, and Professional Standing
Credentials matter because facelift surgery demands nuanced anatomy and meticulous technique. Don’t be shy—ask.
Board certification specificity:
Board certification specificity:
- In the U.S., look for certification by:
- ABPS (American Board of Plastic Surgery)
- ABFPRS (American Board of Facial Plastic and Reconstructive Surgery)
- Outside the U.S., seek the equivalent national board recognized by your country’s medical authority.
- Be cautious: “cosmetic surgeon” is unregulated in many places. Confirm ABMS‑equivalent board status, not just a membership in a “cosmetic” society.
- Verify an ACGME‑accredited residency (plastic surgery or otolaryngology–head and neck surgery) and, when applicable, facial plastic or craniofacial fellowship.
- Ask about annual facelift volume and technique breadth (deep‑plane, SMAS, neck strategies). High, steady volume correlates with mastery.
- Your surgeon should hold active hospital privileges for facelift (rhytidectomy). Hospitals provide ongoing peer review—an extra safety net.
- Surgery should occur in an accredited facility (e.g., AAAASF, AAAHC, The Joint Commission)—proof of anesthesia safety, sterile workflow, and emergency readiness.
- Membership in respected groups—ASPS, The Aesthetic Society, ISAPS, AAFPRS—often reflects commitment to standards and continuing education.
- Ask directly about malpractice history, peer references, and continuing medical education (CME) focused on facelift and facial rejuvenation.
Evaluate the Consultation, Surgical Plan Quality, and Evidence of Results
A great consult is structured and candid. It should feel like a clinical evaluation—not a sales pitch.
Structured assessment:
Structured assessment:
- Expect a thorough facial analysis: cheek (malar) position, jawline/jowl definition, cervicomental angle, platysma bands, skin elasticity, and pigment changes.
- Deep neck considerations—subplatysmal fat, digastric muscle bulk, and submandibular gland visibility—should be addressed because they impact neck outcomes.
- Scar risk should be covered if you have a history of hypertrophic scars or keloids or specific ethnic skin concerns.
- Look for consistent lighting, angles, and backgrounds; 6–12 month postoperative images show durability.
- Find examples that match your age, sex, skin type, and anatomy. Be wary of heavy makeup, filters, or inconsistent lighting.
- Responsible surgeons quote realistic complication ranges and tailor them to you:
- Hematoma: ~2–8% overall; higher in men and with uncontrolled hypertension.
- Temporary nerve weakness (neuropraxia): generally 1–6% transient; permanent injury is rare (<0.5% in published series).
- Skin compromise/necrosis: 1–3%, higher with nicotine exposure.
- Infection: uncommon.
- VTE (DVT/PE): rare in healthy outpatients; risk rises with added factors (immobility, hormone therapy, long‑haul travel).
- Modifiers like smoking/nicotine, aspirin/anticoagulants, uncontrolled blood pressure, and male sex should be discussed specifically.
- Make sure you understand whether the plan is deep‑plane vs. SMAS, anterior vs. lateral platysmaplasty, and any ancillary procedures (fat grafting, submental contouring, skin resurfacing).
- Ask about the revision policy (timing, fees), realistic recovery, and a clear cost breakdown (surgeon, facility, anesthesia, implants/supplies). No surprises.

Assess Safety Infrastructure, Anesthesia, and Perioperative Protocols
Excellence isn’t just technique—it’s systems.
Accredited surgical environment:
Accredited surgical environment:
- Confirm sterile workflow, instrument sterilization (e.g., autoclave logs), and medication safety systems (labeling, reconciliation).
- The facility should have a crash cart, defibrillator, staff with ACLS, and a defined hospital transfer protocol.
- Standardized checklists (e.g., WHO Surgical Safety Checklist) are a good sign of a safety‑first culture.
- Anesthesia should be delivered by a board‑certified anesthesiologist or CRNA under appropriate supervision.
- Discuss options:
- Local anesthesia with oral sedation for limited lifts.
- IV sedation (monitored anesthesia care)—common for many facelifts.
- General anesthesia for complex or combined procedures.
- Airway planning (LMA vs. endotracheal tube) and capnography for sedation cases should be standard. Ask about your ASA classification and intraoperative monitoring.
- Medication management: Coordinate with your prescriber about aspirin, clopidogrel, warfarin, and DOACs; stop bleeding‑risk supplements (ginkgo, ginseng, garlic, high‑dose vitamin E, fish oil) per surgeon guidance.
- Blood pressure control is critical pre‑ and post‑op to reduce hematoma risk.
- Smoking/nicotine cessation is non‑negotiable—ideally 4 weeks before and after. (Nicotine replacement still impairs healing.)
- VTE risk: Your surgeon should use a tool like Caprini scoring to decide on mechanical or chemical prophylaxis.
- Expect precise instructions for dressings, drains (if used), head elevation, and activity.
- Many practices follow ERAS principles (multimodal pain control, antiemetics, early ambulation) to cut opioid use and speed recovery.
- Typical follow‑up cadence: 24–48 hours, 1 week, 2–3 weeks, then 3–6 months and 1 year.
- Ensure after‑hours coverage and a direct line for urgent concerns. Peace of mind matters.
Compare Patient Experience, Ethical Practices, and Practical Logistics
Technical skill is essential—but so are communication, ethics, and logistics.
Interpreting reviews and references:
Interpreting reviews and references:
- Third‑party reviews can help. Look for specifics (how a complication was handled, responsiveness, clarity).
- Ask for patient references who had similar procedures (age, skin type, technique). There’s nothing like candid, real‑world feedback.
- Heavy use of “cosmetic surgeon” without ABMS‑equivalent credentials.
- Unrealistic guarantees, “scarless” promises, “lunchtime facelifts” for substantial aging, or one “proprietary” technique for everyone.
- Hard upselling, sparse or inconsistent photos, refusal to discuss complication management, or lack of hospital privileges.
- Pressure tactics like expiring discounts.
- Comprehensive pricing should include surgeon’s fee, anesthesia, facility fees, and supplies (garments, implants, lab tests).
- U.S. costs vary by region and complexity; a full facelift with neck work and adjuncts often lands in the mid‑five figures. Bargain hunting? Not here—prioritize safety and results.
- Ask about financing options and exact terms, but never at the expense of quality.
- Staying local supports easy follow‑up—and fast management if something like a hematoma appears in the first 24–48 hours.
- Traveling? Plan a 10–14 day local stay and confirm telehealth afterward.
- Discuss emergency coverage, coordination with local providers, and travel restrictions (long flights soon after surgery increase VTE risk).
Practical Questions to Ask During Consultations
Credentials and scope:
- Which board certifications do you hold? Do you have hospital privileges for facelift?
- How many facelifts do you perform annually, and what percentage are deep‑plane vs. SMAS?
- Based on my anatomy, what is your plan for the SMAS, platysma, and neck?
- Will I benefit from adjuncts like fat grafting or laser resurfacing? Why?
- Where will surgery be performed, and what accreditations does the facility hold?
- Who will provide anesthesia? What is my ASA class? How do you mitigate VTE and hematoma risks?
- Can I see unretouched before‑and‑after photos of patients like me, including 6–12 month results?
- What complications should I be most aware of given my health history? How are they handled?
- What’s the expected timeline for bruising, swelling, return to social life, and full result maturation?
- What is your after‑hours coverage and revision policy?
Real‑World Scenarios to Illustrate Decision‑Making
- The marathoner with a long, thin neck: Likely benefits from a deep‑plane facelift with targeted platysma work and conservative fat grafting. The surgeon should discuss submandibular gland visibility and realistic ways to address it.
- The 58‑year‑old with heavy sun damage and jowls: SMAS or deep‑plane for the lower face, plus laser resurfacing or a chemical peel for perioral lines. Emphasis on scar camouflage around the tragus and preserving the sideburn.
- The 65‑year‑old male with hypertension: Tight blood pressure control, careful antiemetic and pain plans to prevent vomiting/bleeding, and a clear discussion of the slightly higher hematoma risk in men.
Putting It All Together: A Shortlist Framework
- Identify 2–4 surgeons with ABPS or ABFPRS certification and active hospital privileges.
- Confirm an accredited facility and robust anesthesia standards.
- Review comprehensive photo portfolios with consistent imaging and long‑term results.
- Compare consultation quality: depth of assessment, candor about risks, and plan specificity.
- Evaluate safety culture: checklists, emergency readiness, and postoperative access.
- Weigh the patient experience: responsiveness, clear pricing, ethical marketing.
- Choose the surgeon whose philosophy fits your goals—and whose practice shows both technical mastery and safety rigor.
Conclusion
Choosing a facelift surgeon is a high‑stakes decision with long‑term implications for your appearance and health. The right surgeon pairs advanced technique with disciplined safety systems, transparent communication, and a tailored aesthetic plan. By confirming board‑specific credentials, assessing case volume and results, scrutinizing anesthesia and facility standards, and insisting on clarity around risks, costs, and follow‑up, you’ll walk in prepared.
A well‑executed facelift should look like you—just more rested, structured, and timeless. With a thoughtful, evidence‑based selection process, that’s not just possible; it’s likely.
A well‑executed facelift should look like you—just more rested, structured, and timeless. With a thoughtful, evidence‑based selection process, that’s not just possible; it’s likely.

Schedule Your Appointment with Dr. Mourad
If you are considering facial plastic surgery and want results that enhance your natural beauty without looking overdone, schedule a consultation with Dr. Moustafa Mourad today. You will receive personal, expert guidance at every step—from your first visit to your final result.
From Our Blog

March 17, 2026 | Dr. Moustafa Mourad | Uncategorized
What Is a Deep Plane Facelift and Why Do Top Surgeons Prefer It?
The deep plane facelift has become the go-to choice for many top facial plastic surgeons—and for good reason. Instead of just pulling skin tight, it works where aging actually happens: in the deeper support layers of the face.
READ THE ARTICLE
March 16, 2026 | Dr. Moustafa Mourad | Uncategorized
What’s the Safest Age to Get a Facelift—and When Is It Too Early?
There isn’t a magic birthday for a facelift. The “safest” age is when your anatomy and skin will clearly benefit more from surgical lifting than from nonsurgical fixes—and when your health makes an elective procedure low risk.
READ THE ARTICLE
March 12, 2026 | Dr. Moustafa Mourad | Uncategorized
Mini Facelift vs. Full Facelift: Technical Differences, Candidacy, and Outcomes
A facelift isn’t one single operation—it’s a range of techniques tailored to how (and where) you’re aging. “Mini facelift” and “full facelift” are common labels, but they point to very different levels of dissection, how deeply tissue is moved, and how much work is done in the neck.
READ THE ARTICLE
March 10, 2026 | Dr. Moustafa Mourad | Uncategorized
Is a Facelift Worth It Compared to Non-Surgical Alternatives? A Clinical, Economic, and Patient-Centered Analysis
Interest in facial rejuvenation has never been higher, but the menu of options—from injectables and energy devices to deep-plane facelifts—can feel overwhelming. Patients often ask a deceptively simple question: is a facelift “worth it” compared to non-surgical treatments?
READ THE ARTICLE